Introduction to Hyperpigmentation and its Prevalence in Skin of Colour
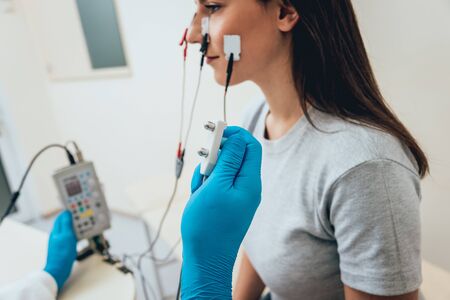
Hyperpigmentation is a common dermatological concern characterised by the darkening of patches of skin due to an excess production of melanin. While it can affect anyone, individuals with skin of colour—including those from Black, South Asian, Middle Eastern, and mixed heritage backgrounds—are disproportionately affected. In the context of contemporary British society, where diversity is woven into the fabric of daily life, the prevalence of hyperpigmentation within these communities cannot be overlooked. Factors such as genetics, inflammation, hormonal changes, and sun exposure play significant roles in its development. For many Britons with skin of colour, hyperpigmentation is not only a cosmetic issue but also one that can impact self-esteem and quality of life. As our understanding of the unique causes and patterns of pigmentation disorders grows, it becomes increasingly clear that solutions must be tailored to reflect the lived experiences and genetic profiles found within Britain’s diverse population. This highlights the urgent need for inclusive research and clinical trials that accurately represent all skin types and backgrounds.
2. Current Gaps in Clinical Research
The issue of underrepresentation in clinical trials for hyperpigmentation solutions remains a persistent challenge, particularly for people of colour living in the UK. Historically, most clinical research has focused on participants with lighter skin tones, often classified as Fitzpatrick skin types I-III. As a result, product efficacy and safety profiles are largely based on data that may not be applicable to those with darker skin (types IV-VI), who often experience different manifestations and underlying causes of hyperpigmentation.
This lack of diversity in clinical studies is problematic for several reasons. Firstly, the biological response to active ingredients—such as hydroquinone, retinoids, or azelaic acid—can differ significantly across various skin types. Secondly, certain side effects, like post-inflammatory hyperpigmentation or irritation, may present more prominently or differently in skin of colour. This means that products deemed “safe” and “effective” for the general population may not yield the same results—or could even cause harm—when used by those with darker skin tones.
Comparing Representation in Clinical Trials
| Skin Type | Percentage Representation in Trials (%) | UK Population Proportion (%) |
|---|---|---|
| Fitzpatrick I-III | 75-90 | 80 (approx.) |
| Fitzpatrick IV-VI | 10-25 | 20 (approx.) |
The Implications for People of Colour in the UK
For people of colour in Britain, this gap translates into a tangible barrier to accessing effective dermatological care. Many available products either lack robust evidence supporting their use in diverse populations or fail to address unique cultural practices and environmental exposures pertinent to UK communities of African, Caribbean, South Asian or mixed heritage. This oversight perpetuates healthcare inequalities and increases the risk of dissatisfaction or adverse outcomes among these groups.
Summary of Key Challenges:
- Limited data on efficacy and safety for skin of colour.
- Poor understanding of unique presentation patterns in hyperpigmentation.
- Lack of culturally tailored advice and treatment options within the NHS and private sector.
Addressing these gaps is essential if we are to provide equitable skincare solutions that genuinely meet the needs of all communities across the UK.

3. The Importance of Representation in Clinical Trials
Ensuring fair and meaningful representation within clinical trials is crucial when developing hyperpigmentation solutions for skin of colour, particularly in the diverse context of the United Kingdom. There are several compelling reasons—ethical, scientific, and societal—that underline why this representation cannot be overlooked.
Ethical Considerations
From an ethical standpoint, it is fundamentally unjust to exclude groups who stand to benefit from medical advances. In Britain’s multicultural society, people with varying skin tones should have equal access to safe and effective treatments. Failing to include individuals from different ethnic backgrounds perpetuates health inequalities and undermines trust in the healthcare system. Inclusion demonstrates respect for all communities, ensuring that no group is left behind as new therapies emerge.
Scientific Validity
Scientifically, a lack of diversity in clinical trials threatens the validity and applicability of results. Skin biology varies widely across ethnicities—factors such as melanin content and the manifestation of hyperpigmentation differ between populations. If studies are conducted primarily on lighter skin types, any conclusions drawn may not translate effectively to those with darker skin tones. This can lead to suboptimal or even ineffective treatment recommendations for large segments of the British population, ultimately compromising public health outcomes.
Societal Impact in the British Context
On a societal level, inclusive research practices foster greater trust and engagement among minority communities. With the UK’s rich tapestry of cultures, people expect to see themselves represented in medical research; it reassures them that their unique needs are recognised and addressed. Moreover, by reflecting the true diversity of Britain within clinical trials, researchers can help combat longstanding disparities in dermatological care, promote social cohesion, and demonstrate a commitment to fairness within the NHS and beyond.
The Path Forward
In sum, meaningful representation within clinical trials is not merely an academic ideal—it is a practical necessity for ethical conduct, scientific rigour, and social responsibility in the UK. For hyperpigmentation solutions to truly serve everyone in Britain, inclusivity must be embedded at every stage of research.
4. Benefits of Inclusive Research for Patients and Practitioners
Inclusive clinical trials, particularly in the context of hyperpigmentation solutions for skin of colour, offer a host of advantages for both patients and practitioners across the UK. By ensuring that diverse populations are represented in research, we can foster better clinical outcomes, more tailored treatments, and heightened trust within our multicultural healthcare environment.
Enhanced Patient Care
When clinical trials actively include individuals with varying skin tones and backgrounds, the findings become directly relevant to those who will ultimately use these treatments. This means therapies are more likely to be effective across the spectrum of patients seen in British clinics. For example, certain hyperpigmentation treatments may interact differently with melanin-rich skin compared to lighter skin, making representation essential for safe and effective care.
Improved Efficacy of Treatments
By embracing inclusivity, researchers gain a clearer understanding of how different skin types respond to specific interventions. This knowledge allows practitioners to select or recommend therapies with greater confidence, knowing that the evidence base reflects the diversity found in the UK. Ultimately, this leads to fewer adverse effects and better overall results for patients from all backgrounds.
Summary Table: Key Benefits of Inclusive Clinical Trials
| Benefit | Impact on Patients | Impact on Practitioners |
|---|---|---|
| Culturally relevant data | Treatments tailored to personal needs | More informed clinical decisions |
| Diverse safety profiles | Reduced risk of side effects | Accurate risk assessment |
| Trust-building | Increased willingness to seek care | Stronger patient-practitioner relationships |
Strengthening Trust in Multicultural Healthcare Settings
The UK is renowned for its cultural diversity, particularly within the NHS and private healthcare providers. When patients see themselves represented in research, it fosters trust in the healthcare system. This is especially important in dermatology, where historical underrepresentation has contributed to hesitancy among people with skin of colour. By prioritising inclusive research practices, clinicians demonstrate respect for every patient’s unique experience and background.
A Pathway to Equitable Healthcare
Ultimately, inclusive clinical trials are not just about science—they are about equity and respect. They set a precedent for how medical research should be conducted in a modern, multicultural Britain, ensuring that every patient receives care grounded in robust and representative evidence.
5. Barriers to Inclusion and How to Overcome Them
Despite growing awareness of the need for diversity in clinical trials, significant barriers persist when it comes to including people with skin of colour in research on hyperpigmentation solutions. In the UK context, these challenges are often nuanced and require specific attention. One of the most prominent obstacles is recruitment. Historically, clinical trials have often been held in locations or through channels that do not reach Black, Asian, and minority ethnic (BAME) communities effectively. There may also be language barriers or a lack of culturally competent communication, leading to lower engagement from these groups.
Mistrust towards medical research represents another substantial barrier. Many people with skin of colour in Britain may carry concerns rooted in past unethical practices or feel that their needs are frequently overlooked by mainstream healthcare. This sense of marginalisation can lead to reluctance in participating in clinical studies, particularly if previous experiences with healthcare have been unsatisfactory or even discriminatory.
To overcome these barriers, researchers must adopt UK-specific strategies focused on building trust and improving accessibility. Community engagement is key; collaborating with local leaders, faith groups, and community organisations can help foster dialogue and raise awareness about the importance of participation in research. Offering study materials and consent forms in multiple languages relevant to British communities—such as Urdu, Bengali, Polish, or Somali—can also make a difference.
Additionally, diversifying the research workforce itself by including more BAME clinicians and researchers can create a more welcoming environment for participants. Training all staff involved in clinical trials on cultural competence ensures sensitivity towards different experiences and perspectives around hyperpigmentation and skincare.
Practical adjustments should also be considered—for instance, holding trial appointments outside of standard working hours or providing travel stipends can remove logistical hurdles that disproportionately affect underrepresented groups. Furthermore, ensuring that results are communicated back to participants—and to their wider communities—in accessible and meaningful ways helps to reinforce trust and demonstrate the value of inclusion.
The collective effort to address these challenges will not only enhance the quality of hyperpigmentation solutions available for skin of colour but also ensure that British healthcare better reflects its richly diverse population.
6. Recommendations for Future Clinical Trials in the UK
To ensure that clinical trials for hyperpigmentation solutions genuinely address the needs of those with skin of colour in the UK, a fundamental shift towards inclusivity is required. Here are practical recommendations for researchers, brands, and policymakers to make this the new standard.
Prioritise Representative Recruitment
Researchers should actively recruit participants from diverse ethnic backgrounds—particularly Black, Asian, and other minority groups who are disproportionately affected by hyperpigmentation but historically underrepresented in dermatological studies. Collaboration with community leaders, local health organisations, and patient advocacy groups can foster trust and encourage participation.
Design Culturally Competent Protocols
Clinical trial protocols must be tailored to account for the unique biological and cultural factors influencing skin conditions in people of colour. This includes using assessment tools validated across different skin tones and ensuring that outcome measures are relevant to all participants. Training research staff in cultural competence is equally essential to minimise unconscious bias throughout the trial process.
Transparent Reporting and Data Sharing
Brands and researchers should commit to publicly reporting participant demographics and stratified outcomes by skin type and ethnicity. Open access to this data empowers clinicians, patients, and policy advocates to make informed decisions about treatment efficacy and safety for diverse populations.
Policy-Driven Incentives for Inclusivity
Policymakers can play a pivotal role by introducing funding incentives, regulatory requirements, or ethical guidelines that prioritise inclusivity in dermatology research. Mandating minimum diversity thresholds for clinical trials receiving public funding will help embed equity into the research infrastructure.
Collaborative Partnerships Across Sectors
The most sustainable progress will come from partnerships between academia, industry, NHS bodies, and community representatives. These collaborations can co-create educational campaigns, develop best practice toolkits, and ensure ongoing feedback from those most affected by hyperpigmentation.
A Commitment to Lasting Change
By implementing these steps, the UK can lead by example in making inclusive clinical trials the norm rather than the exception. Ultimately, such an approach ensures that hyperpigmentation solutions are safe, effective, and accessible for all—regardless of skin colour.